
NEAR Science
NEAR Science (neurobiology, epigenetics, adverse childhood experiences, and resilience) provides a holistic understanding of how trauma and resilience impact health outcomes.
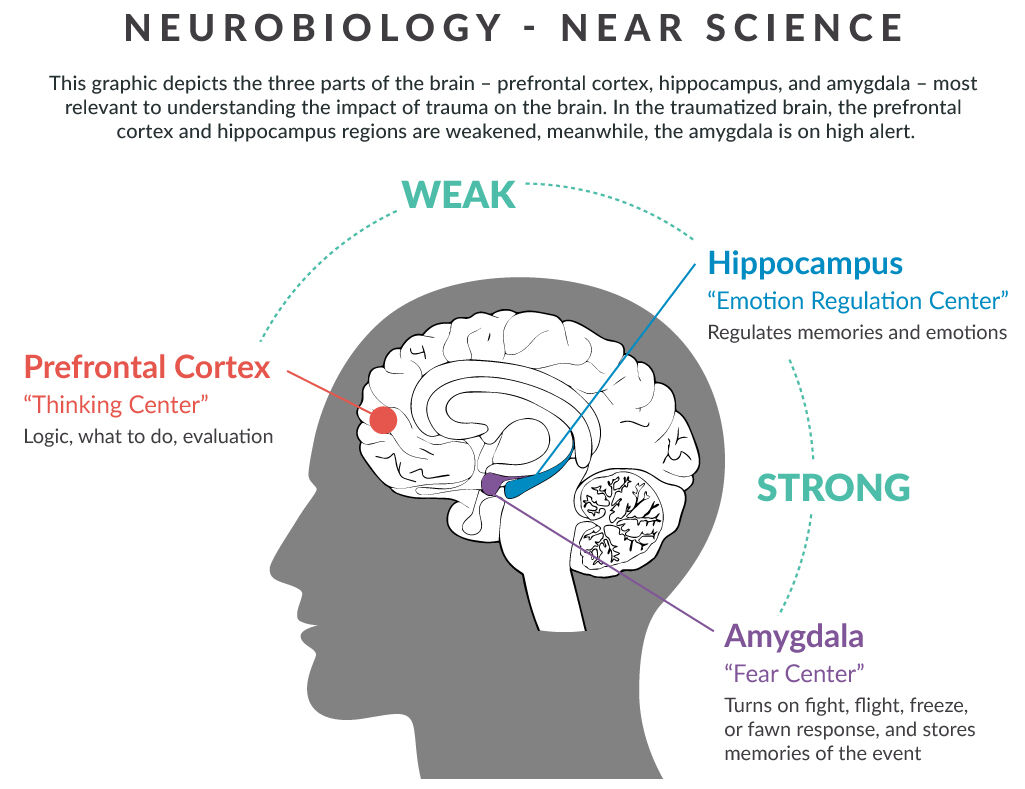
Understanding how the brain is affected by trauma is helpful to implementing trauma-informed approaches and can also help providers better understand the actions and responses of individuals who have experienced trauma. Three primary areas of the brain are impacted by trauma and resilience.
The prefrontal cortex is the “Thinking Center.” When this area of the brain is strong, we can think clearly, make good decisions, and be aware of ourselves and others. After trauma, particularly during childhood, the prefrontal cortex experiences a loss of neuronal integrity and is less able to communicate with other parts of the brain.
The hippocampus is the “Emotion Regulation Center.” When this region is strong, we can manage difficult thoughts and emotions and recall and recognize memories. Individuals who have experienced traumatic stress may experience vivid memories or persistent thoughts that are reminiscent of a trauma. They may have a difficult time distinguishing between a memory and a current threat.
The amygdala, or the “Fear Center,” responds to stress and anxiety and coordinates the behavioral “fight, flight, freeze, or fawn” response. In the traumatized brain, the amygdala is on high alert, often leading to inappropriate, erratic, or defiant behavior as the brain is unable to access the prefrontal cortex and apply logic to a situation.
Traumatic stress responses:
Fight – Temper and angry outbursts, aggressive, dominates and controls, demands perfection from others, pursues power and control, impulsive decision making, critical and rageful
Flight – Feelings of panic and anxiety, obsessive or compulsive disorders, always on the go or staying busy, over worrying, hyperactive, over analytical
Freeze – Depression, dissociation, brain fog, avoiding human contact, detached, struggles with decisions, hibernating, isolation, lifeless
Fawn – People pleasing, co-dependent, lack of boundaries, defers to others to make decisions, avoids conflicts, concerned about fitting in.
Neurobiology Reflection Questions
Use the following reflection questions to incorporate what you have just read in this section into the work you do.
- Which trauma response do you notice as your own default response?
- Which responses do you notice as more prevalent in the individuals you work with?
- How do you respond to other people’s trauma responses?
In the context of trauma, epigenetics is the study of how your behaviors and environment can cause changes that affect the way your genes work. Unlike genetic changes, epigenetic changes are reversible. They do not change your DNA sequence, but they can change how your body reads a DNA sequence. The study of epigenetics offers an important linkage to racialized trauma, critical given the disproportionate impact that HIV has on Black, Indigenous, and other people of color (BIPOC). The centuries of historical and multi-generational trauma experienced by BIPOC are present in the genetic make-up and bodies of today’s BIPOC communities.
Adverse Childhood Experiences {NEAR Science}
Experiences in childhood, both those positive and adverse, have been shown to have lifelong impacts. Adverse childhood experiences (ACEs) refer to experiencing or witnessing abuse, neglect, community violence, racism, poverty, or other dysfunction in a household during a person’s earliest years. ACEs are very common, and especially when compounded, have a strong correlation to health outcomes later in life.
Conversely, positive childhood experiences can be protective factors that occur during childhood and play an important role in contributing to resilience. Positive childhood experiences include the presence of a stable, caring adult (such as a family member, teacher, or mentor), a sense of belonging or connection, and enjoyment in community traditions.
Let community heal community.
Resilience and Healing {NEAR Science}
People can, and do, heal from all kinds of trauma, especially when in relationship with others. Individual resilience refers to a person’s ability to recover from and adapt to difficult experiences. The most common resilience factor is the existence of a caring and supportive relationship. Other resilience factors include the capacity to make and follow through with plans, a positive self-view and confidence in one’s strengths and abilities. It also includes the ability to communicate, problem solve, and the capacity to manage feelings and impulses.
Resilience can be found and built in many ways and many examples of resilience were shared by the TIA Toolkit Advisory Panel. Ryan White HIV/AIDS Program clients demonstrate resilience every time they take their medications or show up for an appointment. Providers can contribute to resilience building by helping clients recognize these strengths, celebrating them, and offering a trusting, supportive relationship.
Resilience Reflection Questions
Use the following reflection questions to think through your own experiences and how to incorporate skills you already have into your workflow.
- Who are the people you rely on when you are having a difficult day/time? What qualities do they possess?
- What qualities do you think you possess that allow for others to rely on you?
- What would you need available to you during your workday or at your organization for it to be a healing space?
- How can you build upon the resilience that the individuals you work with (staff or clients) already possess?